" alt="">
" alt="">
NHS Waiting Times Data Hub

Reviewed by
Peter Rigby - Managing Director of Medical Negligence | Last updated on: 16th July, 2024
Waiting Times Data Hub
- No win No fee
- Not just lawyers - real specialists
- No obligation
- UK's highest-rated medical negligence solicitors
Contents:
- Understanding NHS Waiting Times
- Why Are NHS Waiting Lists So High?
- What Are The Potential Implications Of Longer Patient Waiting Times?
- Specific Area Waiting Times
- A&E Waiting Times
- Ambulance Waiting Times
- Cancer Referral Waiting Times
- Cardiac Care Waiting Times
- Colonoscopy Waiting Times
- Dental Referral Waiting Times
- Surgery And Operation Waiting Times
- MRI Waiting Times
- Expert Comments From Senior Litigation Executive
- Waiting Time Negligence Claims
The NHS is one of the best-performing and most affordable healthcare systems in the world and provides essential medical services to thousands of people across the UK every day. However, one of the persistent challenges facing the NHS is the issue of waiting times for treatments and services. The pressures of higher demand, understaffing, and limited funding are leading to increasing delays.
According to the NHS, patients have the legal right to receive treatment within the set maximum waiting times. These time frames differ for each stage of healthcare and in this data hub we have compiled the maximum times and key statistics for each area of diagnosis and treatment.
Patient waiting times can be the difference between a positive or devastating outcome and it’s important to be aware of the operational standards for each service. Understanding the facts about medical waiting times in the UK can help you know what to expect should you need to use NHS services, and aid us in continuing to support the institution.
Find out if you
have a claim
Take the 10-second claim test
Free Advice
03300 080 352
claim form
We're the highest-rated No Win No Fee medical negligence solicitors on Trustpilot
Understanding NHS Waiting Times
NHS waiting times refer to the duration of time that patients are waiting to receive healthcare services through the National Health Service (NHS) in the UK. These waiting times will vary depending on the type of consultation or treatment that is needed. All waiting times are monitored and the NHS has specific targets that should be followed. Managing waiting times is a big focus for the NHS in order to improve patient outcomes.
If you are referred for a physical or mental health condition within the NHS, you have a legal right to start non-urgent consultant-led treatment, or be seen by a specialist for suspected cancer, within a set amount of time. Your waiting time starts from when the hospital or service receives your referral letter, or when you book your appointment through the referral service. Your waiting time will then end if it is deemed that no treatment is necessary, if you decide that you do not want treatment, or when your treatment begins.
Maximum waiting times for non-urgent referrals
If you are referred for a non-urgent appointment, the maximum waiting time set by the NHS is 18 weeks. This means that you should receive an appointment within 18 weeks from the day of booking your referral appointment.
There are some instances where this 18 week waiting time does not apply, however in general, once you have received a non-urgent referral, you should have an appointment within 18 weeks.
Urgent Suspected Cancer Referral Wait Times
If you have been referred for an urgent cancer check, the cancer should either be confirmed or ruled out within 28 days of the referral. This is part of the Faster Diagnosis Standard (FDS) and this aims to diagnose and treat cancer as early as possible which is extremely vital as the outcomes of cancer are much greater when diagnosed and treated earlier.
Why Are NHS Waiting Lists So High?
NHS waiting lists can be high due to a number of factors including the increased demand for healthcare services, resource constraints and NHS strikes. An ageing population in the UK has led to more people requiring medical attention and additionally, the COVID-19 pandemic had drastic effects on the NHS causing delays in routine treatments and surgeries and creating a backlog.
Professor Sir Stephen Powis who is the NHS National Medical Director said: “Demand for NHS Services across the country remains high – this was a record February for urgent and emergency services, with A&E attendances and ambulance callouts up significantly on pre-pandemic levels.”
However, despite the increase in demand, data shows that the NHS waiting list is continuing to fall with January 2024 data showing that the NHS waiting list is down by 23,761 from the previous month. The number of patients waiting also fell with 6.34 million patients waiting in January 2024 compared to 6.37 million waiting in December 2023.
What Are The Potential Implications Of Longer Patient Waiting Times?
If a patient has received longer waiting times when receiving care from the NHS, it may have serious implications because early detection of an illness or an injury nearly always means a better outcome. So, if there has been a longer wait time for the patient to see their GP or get a referral appointment then this could lead to a delayed diagnosis, and the consequences of a delayed diagnosis can have devastating effects for patients. The implications that this can cause is a delay in treatment which could allow the condition to become worse and the patient may then require further treatments. Overall, longer patient waiting times can have negative consequences for both patients and the NHS.
Specific Area Waiting Times
A&E Waiting Times
A&E departments across England are under increasing pressure, battling against limited NHS funding, chronic understaffing and a higher demand for services: all of which impact patient waiting times.
The operational standard for A&E waiting times is that 95% of patients should be admitted, transferred or discharged within 4 hours of their arrival at an A&E department. This is also known as the ‘four hour performance target’ and was set out in the Handbook to the NHS Constitution. The 95% standard was last met in July 2015.
Accident and emergency waiting times can be critical as delayed treatment can lead to complications and worsening of symptoms.
In February 2024, there was an average of 74,219 A&E attendances per day, however despite this increase in demand, 70.9% of attendances completed their A&E treatment in less than 4 hours, this is an increase compared to 70.3% in January 2024.
This increase is positive but still leaves 29.1% of patients waiting longer than 4 hours to be seen and discharged. Not only does this risk the worsening of their condition, it can also have a harmful effect on a patient’s mental state. Waiting many hours to be seen, whilst in pain, can be stressful and unsettling.
Ambulance Waiting Times
Quick ambulance and 999 response times are crucial, every second counts and can have significant impacts on a patient’s condition.
In January 2024, average ambulance response times for category 2 calls were 40 minutes and 6 seconds, as shown in the graph below. This figure is an improvement from the precious month however it remains over double of the official target which is 18 minutes.
A category 2 call is those classed as a serious condition, such as chest pain or stroke symptoms. The official target for category 2 ambulance waiting times is 18 minutes, but the government set a new target of 30 minutes at the beginning of 2023. This was only met in one month of the year, in January 2023. This is sadly the result of multiple factors contributing to an excessive demand for emergency services.
For the other ambulance categories, waiting times have also failed to meet targets in recent months. The average response time for C1 In April 2024, the most urgent category, was 8 minutes and 10 seconds, longer than the standard of 7 minutes. The C3 ambulance waiting time average in April 2024 reached 1 hour and 42 minutes, this was shorter than the respective average in 2022.
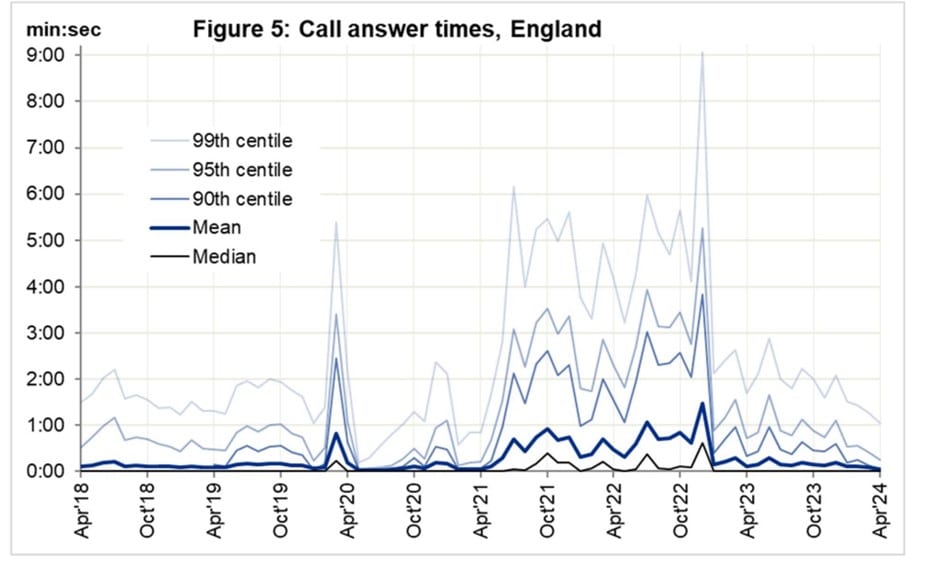
999 call answer times however have seen recent improvement. Emergency services aim to answer 90% of 999 calls within ten seconds. In April 2024, this standard was met, with the average answer time being 3 seconds, shorter than the average of 9 seconds in 2023-24.
Source: NHS
Cancer Referral Waiting Times
Demand for cancer services is at record levels with the number of urgent suspected cancer referrals being at 121% of pre-pandemic levels in December 2023.
Receiving cancer referrals within a timely manner is vital for patients as it means that their treatment can begin as soon as possible. In January 2024, 70.9% of people were told if they had cancer, or if cancer was definitively excluded within the set 28 day waiting time, this is a decrease compared to 74.2% in December 2023.
You can read more about cancer waiting times in our article discussing the current target waiting times and statistics.
Cardiac Care Waiting Times
Delays at any stage of heart care create risk of preventable complications. The British Heart Foundation published findings in March 2024 that the number of people on cardiac waiting lists had risen to 408,061 at the end of January 2024. This is an increase of 2,101 compared to December 2023.
The heart care waiting list was 75% larger than in February 2020 meaning there is an increase of 174,980 people waiting for cardiac care.
They also found that 40% of people on cardiac care waiting lists are waiting over 18 weeks for treatment, where 18 weeks is the maximum NHS-waiting time for non-urgent, consultant-led treatments. Worryingly, these patients are having to endure long waits for life-saving care because of the enduring fallout of Covid-19.
The study did however see improvements in the number of people waiting over a year for time-critical heart tests and treatments. This statistic fell from 10,726 in December 2023, to 10,304 in January 2024.
Colonoscopy Waiting Times
A colonoscopy is a medical diagnosis test, checking the inside of a patient’s bowels. It is used to identify serious conditions such as bowel cancer. NHS England says patients should wait no more than six weeks for tests that can diagnose bowel cancer, and no more than two weeks to see a specialist if they’ve been referred urgently by their GP for suspected bowel cancer.
Bowel Cancer UK found that the number of people on the waiting list for a colonoscopy increased tenfold between 2019 and 2022. Taking a look at recent NHS data, it is promising to see the beginnings of improvements. The proportion of patients waiting over 6 weeks decreased by 4 percent between October 2022 and October 2023, from 39.7% to 35.7%, However this leaves 19,965 people waiting an excessive amount of time for a diagnosis. Early treatment can make a substantial difference on the outcome for a patient.
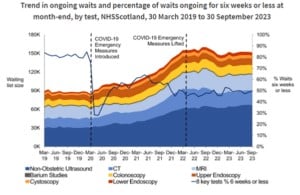
Source: Public Health Scotland
As shown in the graph above, at the end of September 2023, the waiting list for the eight key diagnostic tests sat at 151,651. Although lower than the previous year, this is sadly much higher than prior to the pandemic.
Dental Referral Waiting Times
Failing to receive dental treatment in adequate time can have severe consequences including gum disease and tooth decay. Like other areas of medical treatment, dental referral waiting times have been negatively impacted by Covid-19. Between 2022 and 2023, there were 32.5 million courses of treatment delivered, an increase of 23.2% compared to the previous year. However, this is only two-thirds of the average volumes that were delivered annually in the five years prior to the Covid-19 pandemic.
Under the NHS Constitution, the waiting times for starting non-urgent treatment should not exceed 18 weeks. The target is that 92% should receive treatment in less than this time, but this figure has not been met since March 2016. The number of people on the waiting list for dental treatment has been on the rise since the pandemic, with 20 million dental appointments having been delayed between March 2020 and June 2021.
Waiting times unfortunately deteriorated further in the following year. Data released by NHS England revealed that over 282,000 people were waiting for oral surgery at the end of November 2022, an increase of 87.6 per cent since the beginning of the year.
Looking at 2023, an NHS survey of GP Patient Dental Patients found that 75% of the 759,000 respondents were successful in getting a dental appointment between January and March. To avoid serious dental complications, it is essential that a patient gets diagnosis and treatment as soon as possible. But, success in receiving a dental appointment is dependent on a number of factors. In this same survey, respondents who had not been to the practice before were much less successful in receiving an NHS dental appointment, 33% compared with 84%. Younger adults and ethnic minorities also reported a lower success rate.
For a more in-depth guide to dental negligence, see our Dental Negligence Claims guide.
Surgery And Operation Waiting Times
All operations performed by the NHS should not have a waiting time exceeding 18 weeks. This is pledged in the NHS constitution and the publication also states that if your surgery is cancelled you should be offered another date within 28 days. In addition to these rules, the NHS introduced a new policy in 2014 saying that no one should wait more than 52 weeks. This was designed to prevent very long waits, as the 18 week standard was failing to be met.
Clearly, the emergence of Covid-19 had a major impact on surgical waiting times due to increased burden on the NHS. The 18 week standard was last met in September 2015, and waiting times have since been increasing. Long waits for operations can mean patients suffering with pain for an enduring period, and the possibility of existing conditions worsening.
MRI Waiting Times
Magnetic resonance imaging is a type of scan used to diagnose conditions affecting soft tissue, such as cancers, damaged ligaments and joint injuries. The NHS Constitution aims for patients to receive an MRI scan, for any prospective diagnosis, 6 weeks after their referral.
The average waiting time for an MRI scan is between 6 and 18 weeks in the UK and, in 2023, 26% of patients waited for longer than 6 weeks. This is an encouraging 3% decrease from the previous year. However, 26% equates to 365,990 people having to wait for critical diagnostic tests.
Expert Comments From Senior Litigation Executive
Senior Litigation Executive at Patient Claim Line, Tim Moulton has given expert comments regarding NHS waiting times in the UK: “Longer waiting times in the NHS are a result of wider healthcare concerns and the news surrounding NHS waiting times confirms what I hear from many clients; NHS staff are frequently working against the odds. This inevitably has a detrimental effect on patient safety. However, a number of articles today don’t go far enough in pressing the point that investment in the NHS is lacking. Additionally, I also believe a more in depth and urgent debate needs to be held. Is this due to insufficient funding or a wider issue on how funds are invested?
In short, for everyone who relies on NHS services, this is something that needs to be urgently addressed in detail.”
Waiting Time Negligence Claims
At Patient Claim Line we understand that whilst the NHS are working tirelessly to meet their targets, delays are prevalent in many areas of medical treatment. If you have had a condition worsen due to extended waiting times, you may have a medical negligence claim. A long waiting time can have severe physical and mental implications and we are here to help you pursue financial redress.
We’d advise that you get in touch with our team who will offer friendly guidance for the medical negligence claims process. Our solicitors will provide sensitive and comprehensive advice to help you on your journey to claim compensation for the suffering caused due to longer waiting times within the NHS.
Why Choose Patient Claim Line for your Medical Negligence Claim?
Not just lawyers — medical negligence experts
Patient Claim Line was established in 2014 and consists of a team of medical lawyers specialising in cancer negligence and general medical negligence claims.
At Patient Claim Line we have more than 100 solicitors with a combined experience of over 400 years and they will work on your behalf to achieve the best result possible for you.
It’s not enough to use a solicitor who sometimes covers medical negligence. You need someone who knows this area through and through. That is what the solicitors here at Patient Claim Line do. They deal exclusively in this area of law and are experts in the field.