Hip and knee replacement surgeries continue to be in exceptionally high demand across the NHS, contributing to ongoing long waiting times for patients. While awaiting surgery, many patients experience worsening pain, reduced mobility and a decline in overall health, particularly as joint deterioration progresses without intervention.
Hip and knee replacements remain among the NHS’s highest-volume elective procedures, with tens of thousands of patients referred each year for these life-changing operations.
Quick Statistics:
- NHS target wait: 18 weeks
- Average NHS hip replacement wait: 24-28 weeks
- Average NHS knee replacement wait: 28-29 weeks
Current NHS Waiting Times for Knee & Hip Replacements (2025)
Under NHS England, patients referred for elective treatment such as hip and knee replacement surgery have a legal right to start non-urgent treatment within 18 weeks of referral.
Despite this standard, NHS performance during mid to late 2025 continues to fall short of constitutional targets:
- In 2025, patients awaiting hip replacement surgery in England were waiting an average of approximately 24-28 weeks for treatment.
- Those awaiting knee replacement surgery in 2025 were waiting an average of around 28-29 weeks for treatment.
Hip and knee replacements are among some of the most affected procedures by extended wait times. Orthopaedics remains the speciality with the largest NHS wait list.
Current NHS Elective Procedure Delays (2025)
While the NHS does not publish monthly waiting times by individual procedure in the RTT summary data, orthopaedic services continue to experience some of the longest delays across elective care.
Looking at NHS planned procedure delays, during 2025:
- The most recent January 2026 data shows that around 61.6% of patients in England began treatment within 18 weeks of referral, up from 62% in October 2025, but still a significant shortfall from the NHS standard of 92%.
- The median waiting time across all non-urgent planned procedures in 2025 has remained at approximately 13-14 weeks.
- Around 180,000-200,000 patients were still waiting more than 52 weeks for treatment during late 2025 across all specialities.
This means many patients continue to wait substantially longer than NHS targets, with prolonged periods of pain and restricted mobility.
NHS Waiting List Size ( 2025)
Following sustained pressure from the COVID-19 pandemic and ongoing recovery efforts, the NHS elective waiting list remains historically high:
- By late 2025, there were approximately 7.3 million elective procedures on the NHS waiting list in England.
- This represented around 6.17 million individual patients awaiting consultant-led elective treatment.
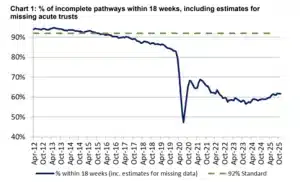
Although long waits have reduced significantly compared to peak pandemic levels, demand for elective and orthopaedic care continues to exceed capacity in many areas. As can be seen in the graph above, the standard of care for elective procedures remains well below the NHS standard.
Why Are Waits So Long?
NHS waiting times for hip and knee replacements are influenced by multiple systemic factors. The most significant drivers of long waits are demand vs capacity, staffing shortages, and pandemic recovery.
Demand vs Capacity
A major reason waiting lists continue to grow is that demand for hip and knee replacements is rising faster than the NHS can deliver treatment.
Why demand is rising:
- An ageing population: Joint degeneration and osteoarthritis become more common as people live longer.
- Increased obesity rates: Excess weight increases stress on joints, raising the need for replacements.
- More referrals from GPs: Greater awareness and improved diagnostic pathways lead to more patients being referred for surgery.
More patients enter the system each year than can be treated, which increases waiting lists and finite resources like operating theatres and post-operation rehabilitation care extends individual wait times.
Staffing Shortages
Staff shortages are a key bottleneck in elective orthopaedic care. Hip and knee replacements require coordinated teams, including Orthopaedic surgeons, Anaesthetists, Theatre nurses, Recovery staff, Physiotherapists and more.
What causes staffing gaps
- Recruitment challenges: Training and recruiting specialist staff takes time and resources.
- Workforce attrition: Retirement, burnout, and staff leaving for private practice or overseas work contribute to shortages.
- High sickness absence rates: Pressures on NHS staff lead to higher absence, reducing capacity.
Even when facilities exist, staffing shortages prevent hospitals from operating at full capacity.
Pandemic Recovery
The COVID-19 pandemic had a major impact on elective care. Many hip and knee replacement surgeries were delayed or cancelled, creating a backlog that the NHS is still recovering from.
Why the backlog persists
- Cancelled surgeries during pandemic peaks created a large volume of delayed cases.
- Priority was shifted to urgent and emergency care, reducing elective capacity.
- Ongoing infection control measures have limited theatre efficiency (eg. longer cleaning and turnaround times).
Why is recovery slow
- The backlog is longer than the system can clear in a short period.
- NHS resources are still stretched by ongoing demand across all specialities.
- New patients continue to join waiting lists while older cases are still unresolved.
Even with improvements, elective waiting lists remain historically high because the system is still catching up.
Impact of Extended Waiting Times for Patients
Waiting longer than clinically necessary for hip or knee replacement surgery can have a significant impact on both physical and emotional well-being. As arthritis and joint damage progress without surgical intervention, patients may experience:
- Increasing joint pain and stiffness, particularly during weight-bearing activities such as walking, standing or climbing stairs, which can severely limit independence and day-to-day function.
- Progressive loss of mobility, leading to muscle wasting around the hip or knee, reduced joint stability and compensatory strain on other joints such as the opposite knee, hips or lower back.
- Reduced activity levels, which may contribute to weight gain and worsening cardiovascular fitness, further increase surgical risk and slow recovery.
- Advanced joint deterioration, which can make hip or knee replacement surgery more complex and potentially reduce the long-term effectiveness of the implant.
- Slower recovery and rehabilitation, as patients who enter surgery with poorer strength, balance and overall health often experience longer hospital stays and reduced post-operative outcomes.
Patients who receive hip or knee replacement surgery earlier, before severe functional decline occurs, are generally more likely to regain mobility, experience pain relief sooner, and achieve better long-term outcomes following surgery.
What This Means
Despite gradual improvements during 2025, NHS waiting times for hip and knee replacement surgery continue to exceed constitutional standards. With only around six in ten patients receiving treatment within the 18-week NHS standard and millions still waiting nationwide, delays remain a significant issue for patients requiring joint replacement surgery.
Reducing waiting times is essential not only to meet NHS targets but also to protect patient outcomes and quality of life. Where delays, cancellations or failures in care have led to avoidable deterioration, patients may wish to seek advice from a medical negligence specialist regarding their options.
Sources
https://www.england.nhs.uk/long-read/reforming-elective-care-for-patients/
https://www.gov.uk/government/publications/the-nhs-constitution-for-england
https://questions-statements.parliament.uk/written-questions/detail/2025-02-10/HL4888/
https://www.kingsfund.org.uk/insight-and-analysis/data-and-charts/waiting-times-non-urgent-treatment
https://www.rcseng.ac.uk/news-and-events/media-centre/press-releases/rtt-jan-2026/
https://www.england.nhs.uk/long-read/operational-performance-update-march-2025

